Google recommended to me this article in Pulse: a publication for GPs. It made me wince quite a bit. A representative of the UK’s “NHS England national infection prevention and control team” was suggesting GPs and others wear surgical masks. The evidence is that FFP2s would be better, offer more protection. I was particularly struck by:
However, she [a “NHS England national infection prevention and control team member”] added that the UK Health and Safety Executive recommends healthcare professionals ‘should not use’ FFP2 masks and that ‘the only requirement to use them’ would be ‘if you couldn’t get FFP3’.
GPs should not routinely use FFP2 as surgical mask gives ‘very good protection’, Pulse, 19th Jan 2022
That is kind of true, the UK’s Health and Safety Executive says:
HSE’s current stance is that where there is a respiratory risk of infection use of FFP3 devices represents best practice, and where these are not available then FFP2 may be an acceptable, pragmatic compromise.
Evaluating the protection afforded by surgical masks against influenza bioaerosols (Research Report 619), Prepared by the Health and Safety Laboratory for the Health and Safety Executive 2008
So, the HSE (who are people in the UK government who understand masks – unlike apparently NHS infection prevention and control) are indeed advising against FFP2s when there is significant risk of infection. They are advising upgrading to a better mask. FFP3s are better than FFP2s. They are not recommending downgrading to the much worse surgical masks, as NHS national infection prevention and control is doing. Odd.
The above quote from the HSE is actually from a report devoted to comparing FFP masks with surgical masks, and this report’s “main findings” are:
This study focussed on the effectiveness of surgical masks against a range of airborne particles. Using separate tests to measure levels of inert particles and live aerosolised influenza virus, our findings show that surgical masks provide around a 6-fold reduction in exposure. Live viruses could be detected in the air behind all surgical masks tested. By contrast, properly fitted respirators [[FFPs] could provide at least a 100-fold reduction
Evaluating the protection afforded by surgical masks against influenza bioaerosols (Research Report 619), Prepared by the Health and Safety Laboratory for the Health and Safety Executive 2008
If you can square this finding from a HSE report with the HSE being invoked to argue against FFPs, and for surgical masks, then comments should be open below. Please let me know. Incidentally, they studied the flu virus not SARS-CoV-2 as this was done in 2008 so pre-pandemic, but flu and COVID-19 seem to spread in very similar ways.
The HSE report is based on some great data:
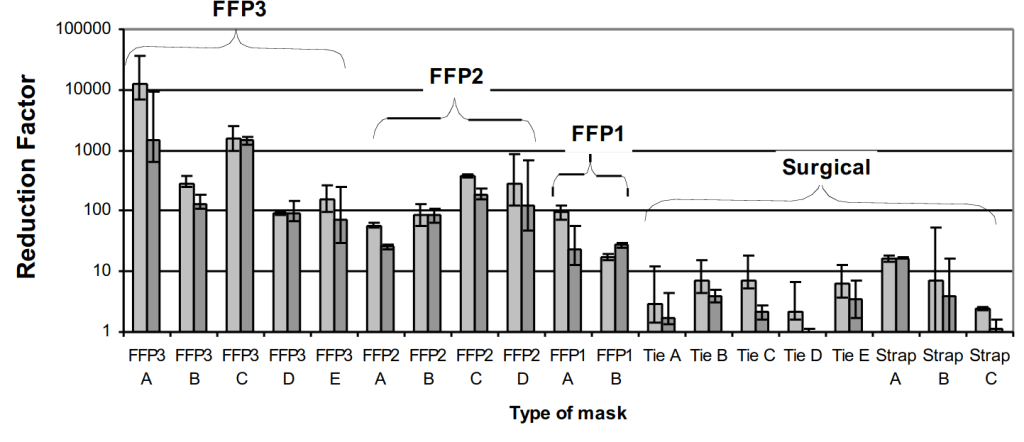
Above, reduction factor is defined so that, for example, a reduction factor of a 100 means that you breathe in 100 times less nasty particles when wearing it. So the higher the better. The FFP naming system is such that FFP3 > FFP2 > FFP1 in terms of protection. The A, B, C, etc denote different masks of same type, and “Tie”, “Strap” denote different ways of keeping the mask place.
On the right hand side are the surgical masks. These offer very variable protection but almost always less than a factor of ten. By contrast, FFP2s reduce exposure by factors around 100*, and FFP3s are better still. Now I have never worn a FFP3 so can’t comment on if they uncomfortable or not, but I wear an FFP2 all the time and they are no more or less comfortable than surgical masks, which I have also worn – although not recently because I decided wearing worse masks was just silly.
Given the well documented chronic shortage of GPs, I think it is everyone’s interest that they don’t get sick. I would say, that this means following HSE’s guidance above, not what NHS infection and control seem to imply is HSE’s guidance.
* These may be under ideal conditions, as others, eg Aaron Collins, find more like factors of 20.
1 Comment